medicine
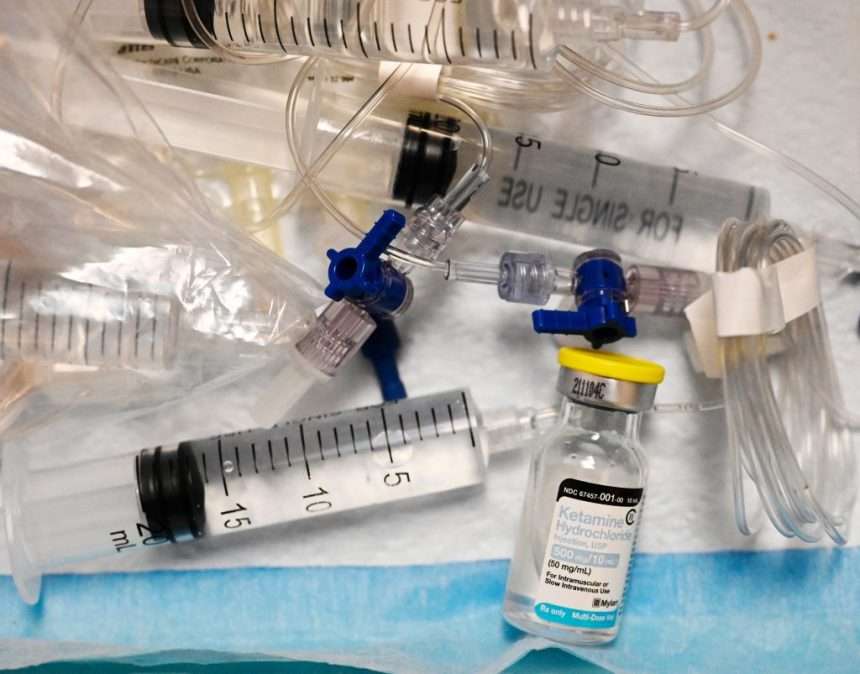
WASHINGTON — As U.S. doctors scale back drug use; opioid painkillers, new options for difficult-to-treat pain are gaining ground.Ketamine is a surgical drug that has been used for decades and is now trendy psychedelic therapy.
Prescriptions for ketamine have skyrocketed in recent years, with commercial clinics and telemedicine services offering ketamine as a treatment for pain, depression, anxiety and other conditions.
Generic drugs are cheap to buy and can be prescribed by most doctors and some nurses, regardless of training.
Research on its effectiveness against pain is limited, leading some experts to worry the U.S. may be at risk. repeated mistakes What caused opioid crisis: overprescription Suspect drug with significant safety and abuse risks.
“With a lack of options for pain, people tend to just grab the next thing that might make a difference,” said Dr. Padma Gulul, a pain expert at Duke University who has studied the use of ketamine. There is,” he said. “When a medical journal publishes a few papers that say, ‘Oh, this is working,’ you end up with rampant off-label use, even though there’s not necessarily any scientific basis behind it.”
Gurule and colleagues tracked 300 patients receiving ketamine at Duke University and found that more than one-third of them had severe symptoms that required professional attention, such as hallucinations, troublesome thoughts, or visual disturbances. reported side effects.
Ketamine also did not reduce opioid prescription rates in the months following treatment, a common goal of treatment, Gul said. Her research is under review for publication in a medical journal.
psychedelic experience
Ketamine was approved more than 50 years ago as a powerful anesthetic for patients undergoing surgery. At lower doses, May produce psychedelic products, an out-of-body experience, became a popular club drug in the 1990s. Recently, this therapy has been adopted for pain as well, and patients are increasingly encountering similar effects.
Daniel Bass, of Southgate, Kentucky, said he found the visual loss “horrifying.” His doctor prescribed his four to six hour IV infusion of ketamine for pain related to a rare bone and joint disease. “I felt like a lab rat,” Bass said, sitting in a bleak hospital room with no stimulation or guidance about the psychological effects of drugs.
Still, he credits the ketamine with relieving his pain during the year he was on IV fluids twice a month.
“No matter how horrible the experience is, if it makes me more functional, I’m going to do it,” Bass said.
Ketamine targets a brain chemical messenger called glutamate, which is thought to play a role in both pain and depression. It is unclear whether the psychedelic experience is part of the drug’s therapeutic effects, but some practitioners believe it is essential.
“We want our patients to feel disconnected and separate from their pain, depression, and anxiety,” says Dr. David Majubi, owner of Ketamine Healing Clinic in Los Angeles. Ta. “If they feel like they’re just sitting in a chair the whole time, we actually give them more chairs.”
Mahjoubi’s practice is typical of a burgeoning industry, offering intravenous ketamine for alcoholism, chronic pain, anxiety, and post-traumatic stress disorder.
Doses of ketamine for these indications are much lower than those used for surgery, but Majubi prefers higher doses for pain rather than psychiatric disorders.
Most insurance companies do not cover non-surgical uses of ketamine, none of which are approved by the Food and Drug Administration, so patients pay cash. Majubi’s background is in anesthesiology, not psychiatry or addiction.
Patients can pay extra for a ketamine nasal spray or tablets to use between infusions. These formulations are also not FDA approved and are compounded by specialty pharmacies.
Mailing ketamine has become a lucrative business in its own right for telemedicine services like Mindbloom, which entered the space after regulators relaxed online prescribing rules during the coronavirus pandemic. It has become.
Pain experts who study ketamine say there is little evidence for these versions.
“There is very little literature on nasal and oral formulations,” said Dr. Eric Schwenk of Thomas Jefferson University. “There’s not really enough evidence to guide you.”
Demand for ketamine has led to prescriptions surging more than 500% since 2017, according to Epic Research, which analyzed trends using a database of more than 125 million patients. While pain was the number one symptom for which ketamine was prescribed each year, depression is rapidly increasing.
prescription boom caused a shortage The amount of ketamine manufactured increased, and sales of the compounded version increased.
There is a lot of evidence that ketamine is used for depression rather than pain. In 2019, the FDA approved a ketamine-related chemical developed by Johnson & Johnson for severe depression. The drug, Sprabat, is subject to strict FDA safety rules about where and how doctors can administer it.
The Pain Society guidelines point to some evidence for the use of ketamine in complex regional pain, a chronic condition that usually affects the extremities. But experts found “weak or no evidence” for ketamine in many more conditions, including back pain, migraines, fibromyalgia and cancer pain.
The “West” of Ketamine Prescriptions
Although the science behind ketamine is unclear, the business model is clear. Doctors can purchase ketamine for less than $100 per vial and charge between $500 and $1,500 per infusion.
The recent boom has been fueled in part by venture capital investors. Another consulting firm is offering to help doctors set up new clinics.
Ketamine Startup’s blog post lists “5 reasons to open a ketamine clinic,” including “I want to be my own boss” and “I want to be in control of my ability to make money.” It contains.
Clinics face increasing competition from telemedicine services such as Mindbloom and Joyous, which connect potential patients with doctors who can prescribe ketamine remotely and mail it to them.
Federal regulators were scheduled to lift the restrictions in May. Coronavirus-era policy allowing online prescriptions High-risk drugs such as ketamine and opioids. But the Drug Enforcement Administration, facing pushback from telemedicine companies and doctors, agreed to extend its flexible approach through 2024.
The current landscape is “the Wild West,” says Dr. Samuel Wilkinson, a Yale University psychiatrist who prescribes both Spravat and ketamine for depression. Doctors in the United States have “considerable discretion” to prescribe drugs for unapproved or off-label uses.
“Some things are good about it and some things are not so good,” he said.
High doses of ketamine can cause bladder damage, which is sometimes seen in people who use it recreationally. Little is known about the neurological effects of long-term use. Ketamine was associated with brain abnormalities in rat studies. FDA Regulatory Note.
last month, FDA warns Doctors and patients oppose ketamine formulations, including lozenges and tablets, arguing that government agencies do not regulate their contents and cannot guarantee their safety. The warning followed a similar advisory last year regarding a nasal spray version of ketamine.
However, most compounding pharmacies are small operations and are supervised by state authorities rather than the FDA.
In April, the Massachusetts Board of Pharmacy flagged the FDA’s warning to local pharmacies, but noted that state officials would not take action to stop “the continued compounding and dispensing of ketamine nasal spray.” .
Similarly, the FDA has little influence over doctors who promote ketamine, even those who make exaggerated or misleading claims.
Pharmaceutical companies are subject to strict FDA regulations regarding how they promote their drugs and must balance risk and benefit information. Those rules do not apply to doctors.
Even if the FDA attempts to regulate dangerous in-office procedures such as: unproven stem cell injectionsthe agency has a mixed track record of success in court.
For now, experts say it is unlikely that regulators will go beyond recent warnings about ketamine off-label.
“There’s an element of whack-a-mole, and it’s essentially beyond regulation,” said Dr. Caleb Alexander, a drug safety researcher at Johns Hopkins University. “These clinics will be a new front that will be difficult to manage and deal with.”
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Science and Education Media Group. AP is solely responsible for all content.
Load more…
{{#isDisplay}}
{{/isDisplay}}{{#isAniviewVideo}}
{{/isAniviewVideo}}{{#isSRVideo}}
{{/isSR video}}