- Antimicrobial resistance (AMR), which the World Health Organization refers to as the “silent epidemic,” is a growing global health crisis that is often overlooked.
- Antimicrobial resistance occurs when microorganisms such as bacteria, viruses, fungi, and parasites develop the ability to persist or even grow despite the presence of drugs designed to kill them.
- To make matters worse, research has shown that climate change is exacerbating antimicrobial resistance in several ways.
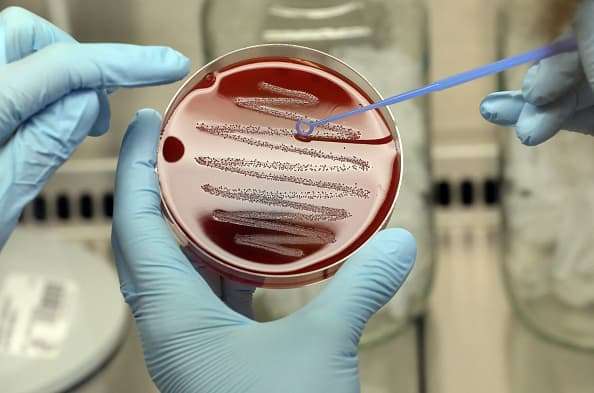
A microbiologist at the Max Planck Institute for Infection Biology prepares a Streptococcus pyogenes bacterial colony on a blood agar plate.
Image Alliance | Image Alliance | Getty Images
actually a favour As one of the major public health threats facing humanity today, it is feared that a warming world will make it more difficult to halt the insidious spread of drug-resistant pathogens.
Antimicrobial resistance (AMR), which the World Health Organization refers to as “The silent epidemicis a growing global health crisis that is often overlooked.
The United Nations health agency had previously announced that antimicrobial resistance is one of the 10 biggest global threats to human health. estimated 1.3 million people die each year directly from resistant pathogens.
This number is on its way toIt rises dramaticallyThe World Health Organization says that if urgent action is not taken, this will lead to higher public health, economic and social costs and push more people into poverty, especially in low-income countries.
Antimicrobials, which include life-saving antibiotics and antivirals, are medicines used to prevent and treat infections in humans and animals. However, it is known that their overuse and misuse is the main driver of the antimicrobial resistance phenomenon.
Antimicrobial resistance occurs when microorganisms such as bacteria, viruses, fungi, and parasites develop the ability to persist or even grow despite the presence of drugs designed to kill them.
People look at a wildfire burning in a forest in Sikorahi, near Alexandroupoli, northern Greece, on August 23, 2023.
Sakis Metrolides | AFP | Getty Images
To make matters worse, research It has been shown that climate change is exacerbating the antimicrobial resistance crisis in several ways.
“Climate change is fundamentally important because of what is happening to our planet, and the problem is that the warmer our temperatures are, the more infectious diseases can be transmitted — and that includes antibiotic-resistant bacteria,” said Tina Joshi, assistant professor of molecular microbiology at Kingdom. United. Plymouth University told CNBC via video.
“Antimicrobial resistant bacteria are known as the silent pandemic,” Joshi said. “The reason it is called the silent pandemic is because no one knows about it — and it is really sad that no one cares.”
A report published by the United Nations Environment Program early this year entitled “Prepare for superbugs“, explains the role of the climate crisis and other environmental factors in the development, spread and transmission of antimicrobial resistance.
These factors include rising temperatures associated with the rate of spread of antibiotic resistance genes among microorganisms, the emergence of antimicrobial resistance due to continued disruption of extreme weather events and increased pollution creating favorable conditions for bugs to develop resistance.
Scientists said earlier this month that an unusual series of global temperature records meant that 2023 was “almost certain” to be the warmest year on record. Extreme heat fueled by the climate crisis, making Severe weather is more frequent and more intense.
It boils down to the fact that it is not economically feasible to actually invest in and develop antibiotics. This is the thing that is shaking up the antimicrobial world.
Tina Joshi
Associate Professor of Molecular Microbiology at the University of Plymouth
Rob Butler, director of the Department of Infectious Diseases, Environment and Health at the World Health Organization in Europe, described antimicrobial resistance as “an extremely pressing global health challenge.”
“It’s a huge health burden and it costs EU member states just somewhere in the region of €1.5 billion ($1.6 billion) a year in health costs but also a loss in productivity. So, it’s a huge challenge,” Butler told CNBC via CNBC. phone.
Butler said he hopes the upcoming COP28 climate conference in the UAE will provide a platform for international policymakers to begin to acknowledge the link between the climate crisis and antimicrobial resistance. The UAE hosts the annual climate summit held by the United Nations from November 30 to December 12.
“The problem is that antibiotics or antimicrobials, of course, are not attractive for industry development. They are expensive, they are very risky – and over the last 20 years we have not seen the development of antimicrobial drugs with sufficient unique properties to avoid resistance.”
“We hear people talking about this ‘silent epidemic,’ but it shouldn’t be silent,” Butler said. “We have to make more noise about this.”
“Can you imagine? [coronavirus] “The pandemic could have been a wake-up call, but we still do not see enough attention to antimicrobial resistance.”
A petri dish comments on bacterial contamination of tray tables at the booth of Polygiene AB, which offers anti-microbial, anti-bacterial and anti-odour technology, at the Aircraft Interiors Expo in Hamburg, Germany, on Wednesday, June 15, 2022.
Bloomberg | Bloomberg | Getty Images
Butler said his greatest interest was perhaps how to motivate industry leaders to tackle antimicrobial resistance, at a time when they are keenly aware that they might be better off investing in other areas of research and development – producing a highly profitable obesity drug, for example.
“For me, this is the thing that keeps me up at night,” Butler said. “I can think about how society might change through trauma to use antibiotics more wisely so that we don’t build antibiotic resistance. But if there’s nothing at all with innovative properties, then we’re kind of lost,” he added. . “That really worries me.”
Joshi of the University of Plymouth echoed this view, describing the antimicrobial resistance diagnostic pipeline as “completely broken” and calling on policymakers to urgently revitalize the process.
“It’s not for profit,” she added. “It boils down to the fact that it’s not economically feasible to actually invest in and develop antibiotics. This is something that is shaking up the antimicrobial world.”
Policymakers risk failing to learn the necessary lessons from the coronavirus pandemic – Thomas Schenker, CEO of Swiss pharmaceutical company Roche, said last month – adding that this could have serious implications for the antimicrobial resistance health crisis.
“I don’t think we learned the lessons we should have learned in the last pandemic, and I don’t think we’re better prepared for the next one,” Schenker told CNBC’s “Squawk Box Europe” on Oct. 19. .
He continued: “I think it is important that we learn these lessons, and do what we need to do to prepare for the next pandemic to come.”
“One of my concerns is that antibiotic-resistant bacteria could be this pandemic. However, we need to focus on preparing for such situations in the future.”