Clinicians in the United States may be overprescribing topical antifungals for skin infections, potentially exacerbating the growing problem of drug resistance. According to new research.
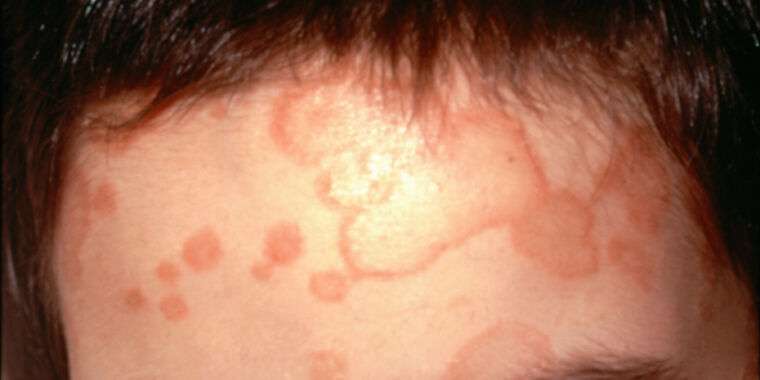
Last year, New York dermatologists reported the nation’s first case of a newly emerging skin fungus that is highly contagious and resistant to common antifungal treatments. It appears that a growing silent community is behind these unrelated incidents. Overall, cases of drug-resistant fungal skin infections (also known as ringworm) have been confirmed in at least 11 states in the United States so far.
With bacterial resistance on the rise, researchers at the Centers for Disease Control and Prevention took a closer look at how U.S. clinicians prescribe topical antifungal drugs. As with antibiotics and bacterial infections, overuse of antifungal drugs can promote the development of resistance. Also, without a diagnosis, it is very difficult to properly diagnose a skin infection. A 2016 research study found that even board-certified dermatologists Mistakes often occur when trying to identify skin infections by sight alone.
As a first step to assess the situation, CDC researchers looked at data on prescriptions written for 48.8 million Medicare Part D beneficiaries in 2021. During the year, clinicians prescribed 6.5 million topical antifungal treatments. That’s enough prescriptions for about 1 in 8 Medicare Part D beneficiaries to receive an antifungal drug.
Among the entire Medicare prescriber data set, there were just over 1 million prescribing clinicians, but only about 131,000 of them prescribed topical antifungals. When these prescribers were ranked by the amount of antifungal treatments they prescribed, the top 10 percent of 13,106 prescribers accounted for approximately 45 percent of all antifungal prescriptions written that year, or a total of 650 prescriptions. This accounted for 2.9 million of the million cases.
problem prescriber
Most prescriptions for antifungal drugs, a topic of the year, are written by primary care physicians, with approximately 40% of prescriptions written by primary care physicians. This was followed by nurse/physician assistants, dermatologists, and podiatrists.
The most common prescriptions were ketoconazole, nystatin, and clotrimazole betamethasone dipropionate, a combination drug containing an antifungal and corticosteroid. The latter is of particular concern as this combination is thought to be a factor in drug resistance.
Data suggests that some healthcare providers may be overprescribing antifungal drugs, but researchers believe that some antifungal drugs are particularly prone to developing resistance. did not have diagnostic data for the cases. Therefore, we could not know how many antifungal prescriptions were supported by diagnostic tests confirming fungal infection. That said, another limitation of this study is that it did not capture the use of over-the-counter antifungal drugs. Therefore, antifungal use among Medicare beneficiaries may be underestimated.
The authors note that this study is a preliminary step toward improving antifungal management. However, “substantial prescriptions of topical antifungals and antifungal corticosteroids among Medicare Part D beneficiaries are occurring in a setting where resistant infections are emerging.” ,” the authors conclude, “highlighting the need to evaluate current practices of topical antifungal use.” Clinicians should “be prudent” and confirm the diagnosis of a skin fungal infection if possible, he cautions.