Once again, it appears that many people in the Bay Area are infected with COVID-19, and data suggests the rise in cases is not merely anecdotal.
In Santa Clara County, Wastewater samples show high levels of the virus again in the Sunnyvale, Palo Alto and San Jose watersheds.After a spring lull, the number of cases hit its lowest in more than two years. The positivity rate has also increased significantly in recent weeks..
Dr. John Swartzberg, clinical professor emeritus at the University of California, Berkeley School of Public Health, has noticed the increase from anecdotes among friends and colleagues and from the data. But is there any good news?
“Far from approaching winter, it’s no higher than it was on this day a year ago,” he said. Virus indicators will be lower in 2024 than they will be in 2023, he said. And California saw its lowest death toll on record this spring, with the state seeing no COVID-19 deaths for the first time in more than four years.
While public health officials no longer release the number of COVID cases detected each day, as they did during the height of the pandemic, local officials continue to track COVID levels in wastewater, which can be an early warning of virus surges and subsidence. The state health department also continues to track the percentage of people tested for the virus statewide that test positive. Both metrics have shown increases in recent weeks. New variants emerged, turning a slow spring surge in COVID-19 infections into a full-blown summer surge..
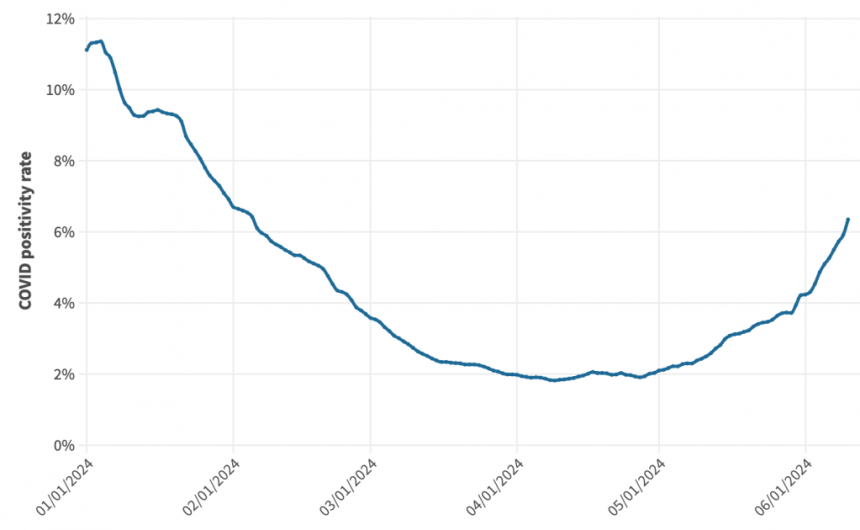
California’s positivity rate had dipped to nearly 2% throughout April, but began to rise again in May. On May 1, the positivity rate was 2.1%, and by June 1, it was over 4%. In this week’s update posted Friday, the positivity rate continued to rise, increasing nearly 2% to 6.4% on June 10.
Schwartzberg acknowledged that while infection rates are rising, the situation is much better than in past years, but he said it’s “deeply disappointing” that older and more vulnerable people are not getting the latest vaccines introduced last fall or the recommended booster shots.
“Fifty-five percent of the population over 65 are not taking advantage of something that is likely to prevent a bad outcome, even though they are actually at high risk of having a bad outcome,” he said.
That’s consistent with what Dr. Peter Chin-Hong, an infectious disease professor and professor of medicine at the University of California, San Francisco, has seen in comparing recent hospital case counts with previous surges.
“In 2020, we would be talking about intensive care beds. In 2022, we would be talking about hospitalizations. And now in 2024, we’re talking about urgent care, emergency department visits, people recovering at home,” he said.
So what about those who are still infected and hospitalized with COVID-19? “They’re older, they’re immunocompromised, and in my experience, none of them have been up to date on the vaccine,” Chin-Hong points out. “They’re not anti-vaccination or anything like that. They’re just feeling safe right now, and that’s what worries me.”